Explore oral cavity anatomy and function, including key structures, roles in speech and digestion, clinical relevance, and why it matters for dental professionals.
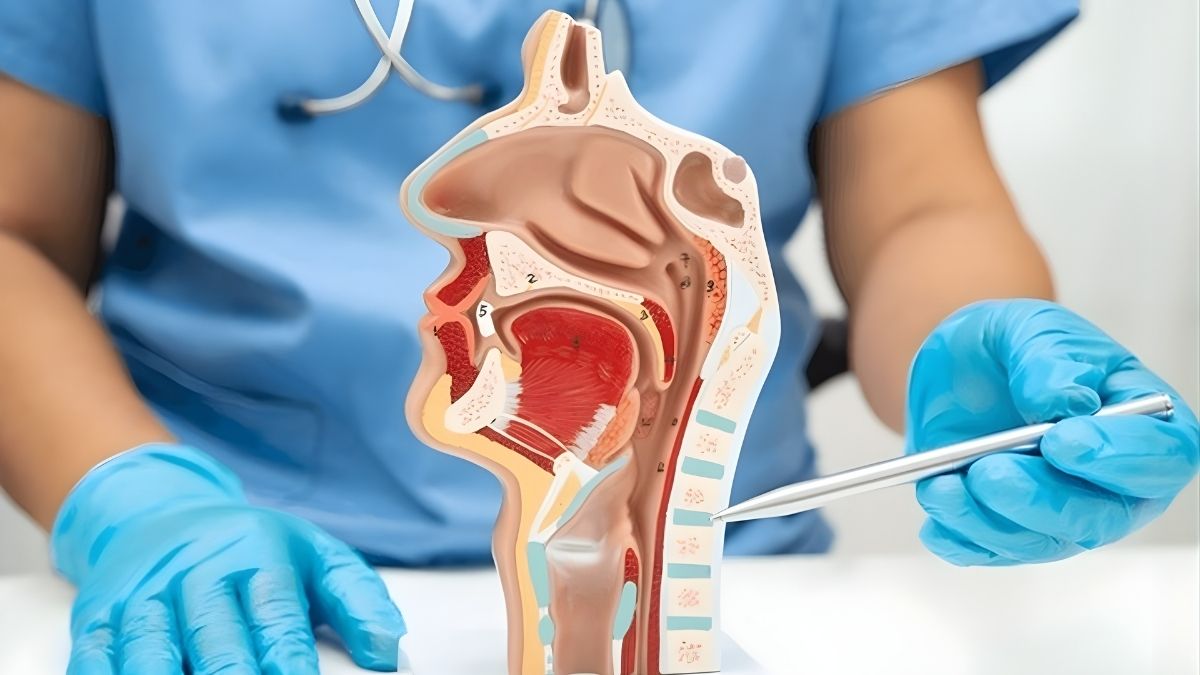
Table of contents [Show]
- Understanding the Oral Cavity: Definition and Clinical Importance
- Main Regions of the Oral Cavity
- Key Anatomical Structures of the Oral Cavity
- Innervation and Blood Supply of the Oral Cavity
- Major Functions of the Oral Cavity
- Common Oral Cavity Disorders and Their Clinical Relevance
- Why Oral Cavity Knowledge Matters Across Dental Specialties
- Oral Cavity Structures and Their Primary Functions
- What This Means for Dental Practices and Lab-to-Lab Workflows
- Key Takeaways
- References
The oral cavity is far more than the opening of the digestive tract. It is a highly specialized anatomical system that supports mastication, speech, taste, respiration, facial expression, and oral protection. For dental professionals, understanding the structure and functions of the oral cavity is foundational to diagnosis, treatment planning, restorative success, and long-term oral health outcomes.
Below is a practical, clinically relevant overview of oral cavity anatomy, its key structures, major functions, and why this knowledge matters across dentistry, prosthodontics, implantology, and lab-to-lab workflows.
Understanding the Oral Cavity: Definition and Clinical Importance
The oral cavity, also called the mouth or buccal cavity, is the first part of the digestive system and the entry point for both food and air. It also plays an essential role in phonetics, swallowing, sensory perception, and immune defense.
From a dental perspective, the oral cavity is not just a space. It is a functional unit where hard tissues, soft tissues, muscles, nerves, blood vessels, and salivary structures work together. Every restoration, denture, implant case, occlusal adjustment, and periodontal treatment depends on a precise understanding of this environment.
Why It Matters in Dentistry
- It influences occlusion, mastication, and bite force distribution.
- It determines speech adaptation for prosthetic and restorative cases.
- It affects salivary balance, lubrication, and tissue tolerance.
- It guides implant placement, removable prosthetic design, and restorative contours.
- It supports the diagnosis of oral disease, pathology, and functional disorders.
In practice, this means that oral cavity anatomy is not theoretical knowledge. It directly affects fit, function, esthetics, and patient comfort.
Main Regions of the Oral Cavity
The oral cavity is commonly divided into two major anatomical regions. This distinction is especially important in clinical examination and prosthetic planning.
Oral Vestibule
The oral vestibule is the space between the inner surfaces of the lips and cheeks and the outer surfaces of the teeth and gingiva. This area acts as a transitional zone between the external environment and the inner oral space.
Clinical Significance of the Oral Vestibule
- Important for flange design in removable prosthetics.
- Relevant for muscle attachments that affect denture stability.
- Influences food retention, oral hygiene access, and speech movement.
- Plays a role in facial support and esthetic appearance.
Oral Cavity Proper
The oral cavity proper is the internal space located within the dental arches. It is bounded by the teeth and gingiva, the hard and soft palate, the floor of the mouth, and the tongue.
This is the primary functional chamber for chewing, bolus formation, swallowing initiation, and articulation.
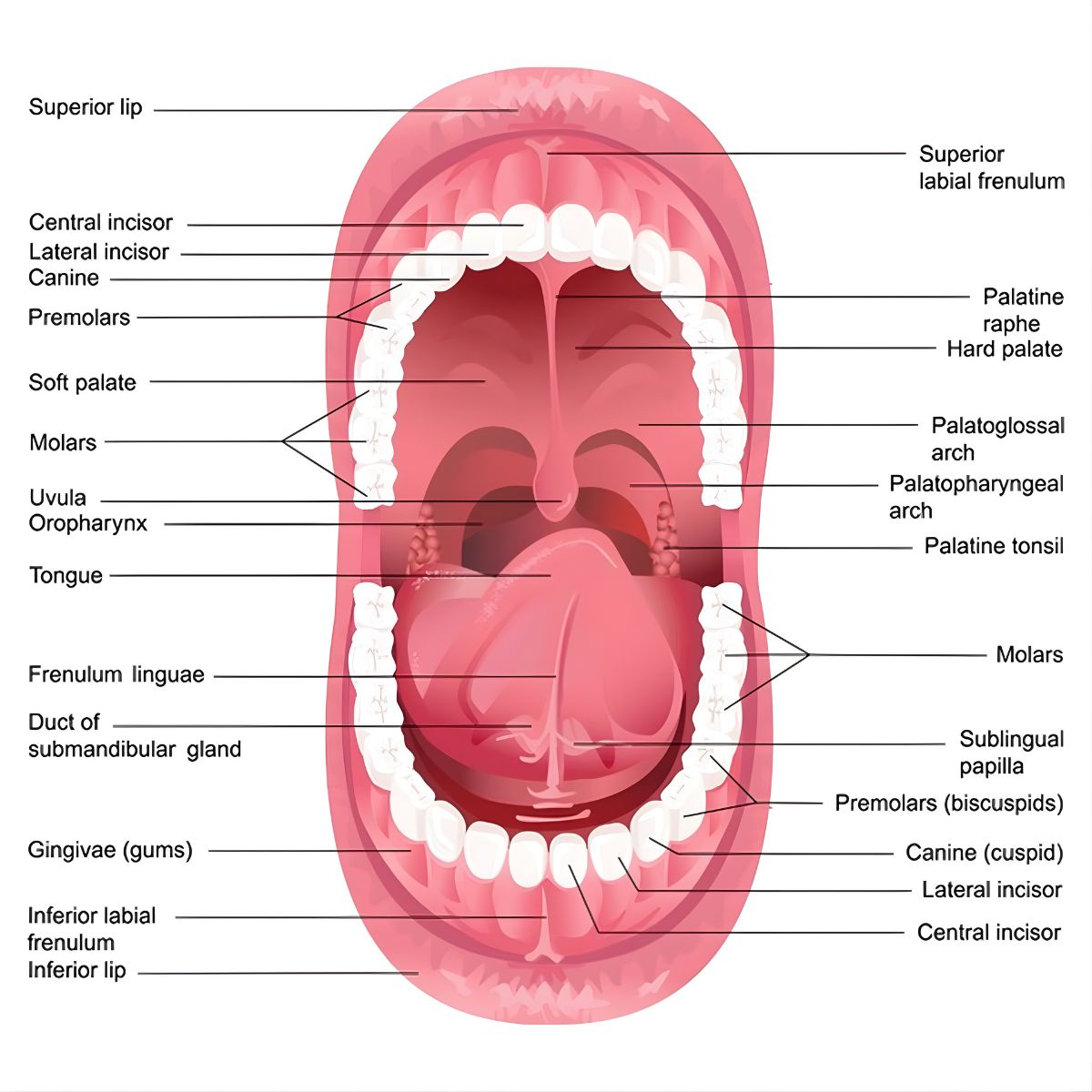
Key Anatomical Structures of the Oral Cavity
Each structure in the oral cavity contributes to one or more physiological and clinical functions. Understanding these structures as an integrated system is essential.
Lips and Cheeks
The lips and cheeks form the outer boundaries of the mouth and contribute to both function and facial expression.
Their Main Roles Include
- Helping with food intake.
- Maintaining the bolus during mastication.
- Supporting speech articulation.
- Contributing to facial esthetics.
- Assisting with oral sealing.
Two important muscles include the orbicularis oris, which controls lip movement and closure, and the buccinator, which helps keep food between the occlusal surfaces during chewing.
For prosthetic and restorative work, lip support and cheek dynamics strongly affect phonetics, smile design, and denture flange contour.
Teeth
Teeth are the principal hard structures of the oral cavity and are essential for mechanical digestion.
Types of Teeth and Functions
- Incisors cut food.
- Canines tear food.
- Premolars crush and transition food.
- Molars grind food.
Basic Tooth Structure
- Enamel: outer mineralized layer.
- Dentin: supportive internal hard tissue.
- Pulp: neurovascular center.
- Cementum: covers root surfaces and supports periodontal attachment.
For dental labs, tooth anatomy affects cusp-fossa relationships, occlusal morphology, interproximal contact design, and the functional anatomy of crowns and bridges.
Tongue
The tongue is a muscular organ covered by mucosa and specialized papillae that contain taste receptors.
Key Functions of the Tongue
- Manipulates food during mastication.
- Forms and positions the bolus for swallowing.
- Supports speech production.
- Detects taste.
- Helps maintain oral cleansing.
The tongue also affects denture stability, lingual flange extension, and speech adaptation in removable and fixed prosthetics.
Palate
The palate forms the roof of the mouth and separates the oral cavity from the nasal cavity.
It Has Two Parts
- Hard palate: anterior bony portion.
- Soft palate: posterior muscular portion.
Functional Importance
- Separates oral and nasal spaces.
- Contributes to speech resonance.
- Helps direct food during swallowing.
- Provides support and coverage area for maxillary dentures.
In prosthodontics, palatal anatomy is critical for major connector design, denture retention and suction, and speech comfort and adaptation.
Salivary Glands
The major salivary glands include the parotid glands, submandibular glands, and sublingual glands. Saliva is essential for oral health and function.
Functions of Saliva
- Lubricates oral tissues.
- Begins carbohydrate digestion through amylase.
- Supports taste sensation.
- Protects against microbial overgrowth.
- Helps buffer acids.
- Improves swallowing and tissue comfort.
Reduced salivary flow can severely affect denture tolerance, caries risk, soft tissue health, and speech and mastication efficiency.
Gingiva and Periodontium
The gingiva surrounds the teeth and provides a protective soft tissue seal. The periodontium includes the gingiva, periodontal ligament, cementum, and alveolar bone. Together, these tissues support the teeth and absorb functional forces.
Why This Matters Clinically
- Healthy periodontal support is essential for restoration longevity.
- Margin design must respect soft tissue architecture.
- Implant and crown outcomes depend on biologic and structural support.
- Removable and fixed prosthetics must distribute forces carefully.
Oropharyngeal Connection
The oral cavity opens posteriorly into the oropharynx through the oropharyngeal isthmus. This opening allows the passage of food toward the digestive tract and air toward the respiratory tract.
This connection is especially relevant for swallowing coordination and airway-related considerations.
Innervation and Blood Supply of the Oral Cavity
The oral cavity is highly vascularized and richly innervated, which explains its sensitivity, healing capacity, and complex functional control.
Innervation
Several cranial nerves contribute to oral function:
- Trigeminal nerve (CN V): sensation and mastication.
- Facial nerve (CN VII): facial expression and some taste functions.
- Glossopharyngeal nerve (CN IX): taste and sensory roles in the posterior tongue and pharynx.
- Hypoglossal nerve (CN XII): tongue movement.
Clinical Relevance
These neural pathways are essential for chewing, swallowing, speech, sensory detection, pain perception, and reflex coordination.
Blood Supply
The oral cavity receives arterial blood mainly from branches of the external carotid artery, especially the facial artery, lingual artery, and maxillary artery.
Venous drainage occurs mainly through the facial vein and pterygoid venous plexus.
This vascular network supports tissue nourishment, healing, inflammation response, and surgical planning considerations.
Major Functions of the Oral Cavity
The oral cavity performs multiple overlapping functions. In dentistry, these functions should be understood not in isolation, but as part of a coordinated oral system.
Digestion
The oral cavity begins the digestive process through food intake, mechanical breakdown by teeth, mixing with saliva, and bolus formation. Salivary amylase initiates carbohydrate digestion even before food reaches the stomach.
Speech and Articulation
Speech depends heavily on the coordinated movement of the tongue, lips, teeth, hard palate, and soft palate. This is why changes in tooth position, vertical dimension, palatal contour, and incisal edge location can directly alter phonetics.
Taste Perception
Taste buds, especially on the tongue, allow detection of sweet, salty, sour, bitter, and umami. Taste contributes to appetite, food choice, and sensory awareness.
Respiration
Although the nose is the primary airway, the oral cavity serves as a secondary respiratory passage, especially during exertion or nasal obstruction.
Protection
The oral cavity helps protect the body through intact mucosal barriers, salivary cleansing, immune components in saliva, and sensory warning systems for heat, pain, and texture.
Communication and Expression
The mouth is central to verbal communication, smiling, emotional expression, and social interaction. This makes oral rehabilitation not just functional, but deeply connected to confidence and quality of life.
Thermal and Tactile Sensation
The oral tissues are highly sensitive to temperature, pressure, texture, and pain. This sensory feedback protects against injury and helps assess food safety and consistency.
Common Oral Cavity Disorders and Their Clinical Relevance
A healthy oral cavity depends on the integrity of both hard and soft tissues. Several disorders can disrupt oral function and treatment outcomes.
Common Conditions Affecting the Oral Cavity
- Dental caries: caused by acid-mediated demineralization of tooth structure and may compromise function, esthetics, and restorative prognosis.
- Periodontal disease: includes gingivitis and periodontitis and can damage supporting tissues, leading to tooth mobility or loss.
- Oral cancer: often associated with tobacco, alcohol, and other risk factors, requiring early recognition and timely referral.
- Xerostomia: reduces lubrication and increases caries and mucosal irritation risk, while making removable prostheses less comfortable.
- Malocclusion: affects bite efficiency, esthetics, speech, and restorative planning.
- Cleft lip and palate: congenital structural anomalies with major effects on feeding, speech, and craniofacial development.
- Temporomandibular disorders: can influence jaw function, occlusion, and patient comfort during treatment.
Why These Conditions Matter to Dental Labs and Clinicians
These disorders influence impression accuracy, occlusal registration, prosthetic fit, material selection, soft tissue response, and long-term maintenance.
A restoration that looks excellent on the model but ignores the oral environment may fail clinically despite strong esthetics.
Why Oral Cavity Knowledge Matters Across Dental Specialties
A detailed understanding of oral anatomy supports nearly every field in dentistry.
Restorative Dentistry
It helps create restorations that are functional, esthetic, and biologically compatible while guiding contour, contact, emergence profile, and occlusion.
Prosthodontics
It is essential for the design of crowns, bridges, dentures, and implant-supported restorations, supporting better adaptation to soft tissue, occlusal forces, and speech patterns.
Implant Dentistry and Oral Surgery
It is necessary for safe placement, angulation, prosthetic planning, and anatomical risk assessment.
Periodontics
It improves diagnosis and management of tissue support and biologic width considerations.
Orthodontics
It supports diagnosis of arch relationships, tooth movement, and functional bite issues.
Pediatric Dentistry
It requires knowledge of tooth development, eruption patterns, and changing oral anatomy.
Oral Cavity Structures and Their Primary Functions
Below is a quick-reference summary connecting anatomy to function.
| Structure | Primary Role | Dental Relevance |
|---|---|---|
| Lips and cheeks | Food control, speech, facial expression | Affects esthetics, phonetics, flange design |
| Teeth | Cutting, tearing, grinding | Determines occlusion, restoration design, mastication |
| Tongue | Taste, speech, bolus control | Influences phonetics, denture stability, lingual contours |
| Palate | Separation of oral and nasal cavity, speech, swallowing | Important for maxillary prosthetics and speech adaptation |
| Salivary glands | Lubrication, digestion, buffering, protection | Impacts caries risk, tissue comfort, prosthesis tolerance |
| Gingiva and periodontium | Support and protection of teeth | Critical for margins, stability, and long-term success |
This table reflects a core principle in dentistry: structure drives function, and function strongly influences clinical success.
What This Means for Dental Practices and Lab-to-Lab Workflows
For dental practices, a strong understanding of oral cavity anatomy improves diagnosis, treatment planning, patient communication, and long-term case success.
For dental laboratories, especially in lab-to-lab outsourcing, this knowledge helps ensure that restorations are not just fabricated accurately, but designed in line with real intraoral function.
Relevance to XDENT LAB
As a Vietnam dental lab specializing in lab-to-lab full service, removable solutions, and implant cases for the U.S. market, XDENT LAB operates in areas where oral anatomy and function directly influence product quality.
This is especially important in removable prosthetics, where vestibular depth, tongue space, palate form, and soft tissue support affect retention and comfort; in implant restorations, where occlusion, emergence profile, tissue relationships, and anatomical precision matter greatly; and in consistent outsourced production, where anatomical understanding supports predictable outcomes at scale.
For practices seeking quality, compliance, and consistency, working with a lab that understands not only the restoration, but also the oral environment it must function within, creates a meaningful clinical advantage.
Key Takeaways
The oral cavity is a multifunctional anatomical system that supports digestion, speech, taste, respiration, protection, and facial and social communication.
Its major structures, including the lips, cheeks, teeth, tongue, palate, salivary glands, gingiva, and periodontium, work together in a dynamic and clinically significant way.
For dental professionals, this knowledge is essential across restorative dentistry, prosthodontics, implantology, orthodontics, periodontics, oral surgery, and pediatric care.
Better understanding of oral cavity anatomy leads to better treatment decisions, better prosthetic design, and better patient outcomes.
References
- Anatomy, Head and Neck, Oral Cavity (Mouth) – NCBI
- Mouth Anatomy – Oral Cavity Proper – Medscape
- The Oral Cavity – TeachMe Anatomy
- Oral Cavity – Medires Online
XDENT LAB is an expert in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable & Implant, meeting U.S. market standards – approved by FDA & ISO. Founded in 2017, XDENT LAB has grown from local root to global reach, scaling with 2 factories and over 100 employees.. Our state-of-the-art technology, certified technicians, and commitment to compliance make us the trusted choice for dental practices looking to ensure quality and consistency in their products.
Our commitments are:
100% FDA-Approved Materials.
Large-Scale Manufacturing, high volume, remake rate < 1%.
2~3 days in lab (*digital file).
Your cost savings 30%.
Uninterrupted Manufacturing 365 days a year.
Contact us today to establish a strategy to reduce operating costs.
--------❃--------
Vietnam Dental Laboratory - XDENT LAB
🏢 Factory 1: 95/6 Tran Van Kieu Street, Binh Phu Ward, Ho Chi Minh City, Vietnam
🏢 Factory 2: Kizuna 3 Industrial Park, Can Giuoc Commune, Tay Ninh Province, Vietnam
☎ Hotline: 0919 796 718 📰 Get detailed pricing
Share this post:





