A practical Kennedy Classification guide: clearly explaining Class I, II, III, and IV cases and adopt dental laboratory frameworks—lab‑to‑lab consistency with XDENT LAB.
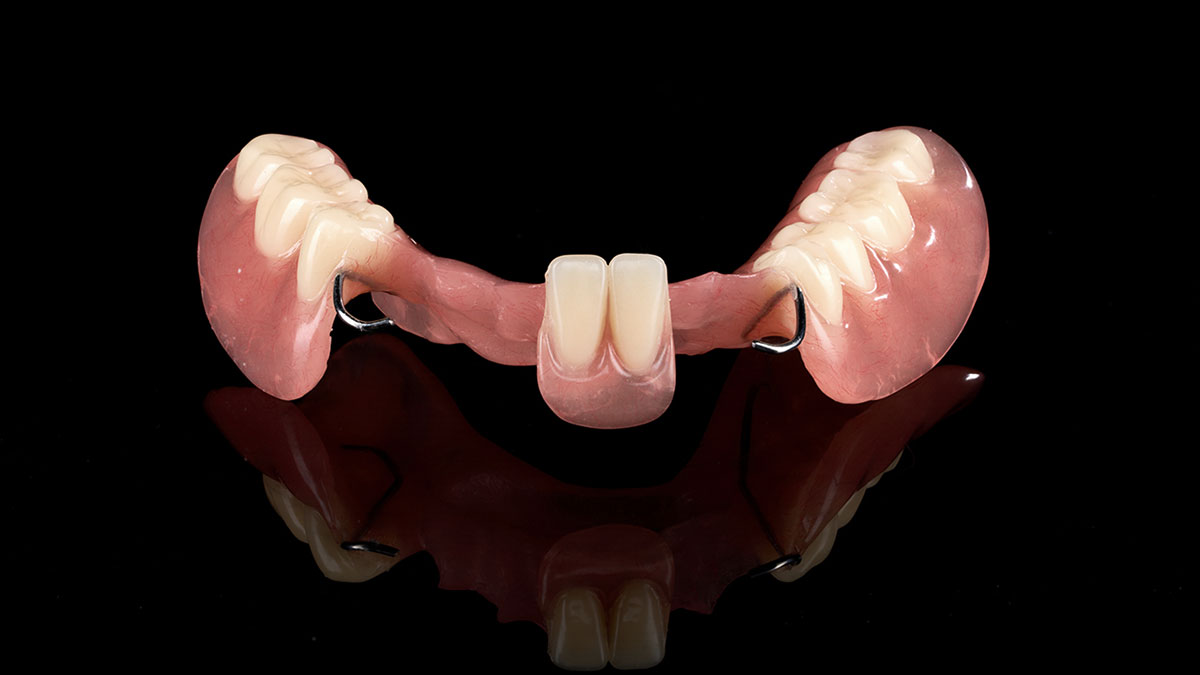
Table of contents [Show]
- Overview
- The Kennedy Classification System
- Prevalence & Clinical Significance
- Biomechanics That Drive Design
- Design Playbooks by Class
- Digital Workflows & Materials
- Implant-Assisted Kennedy Dentures (Classes I & II)
- Comparative Snapshot
- Maintenance & Long-Term Success
- QA & Risk Control for Clinics and Labs
- Where XDENT LAB Fits
- Key Takeaways
Overview
Kennedy dentures are removable partial dentures (RPDs) planned and designed using the Kennedy Classification, a century-old system that remains the global standard for categorizing partial edentulism. Its staying power comes from clinical clarity: the classification mirrors how forces travel through teeth, mucosa, and frameworks, and it supports consistent communication between dentist and lab. Modern advances—implants, digital design, high-performance polymers—augment, rather than replace, Kennedy principles.
The Kennedy Classification System
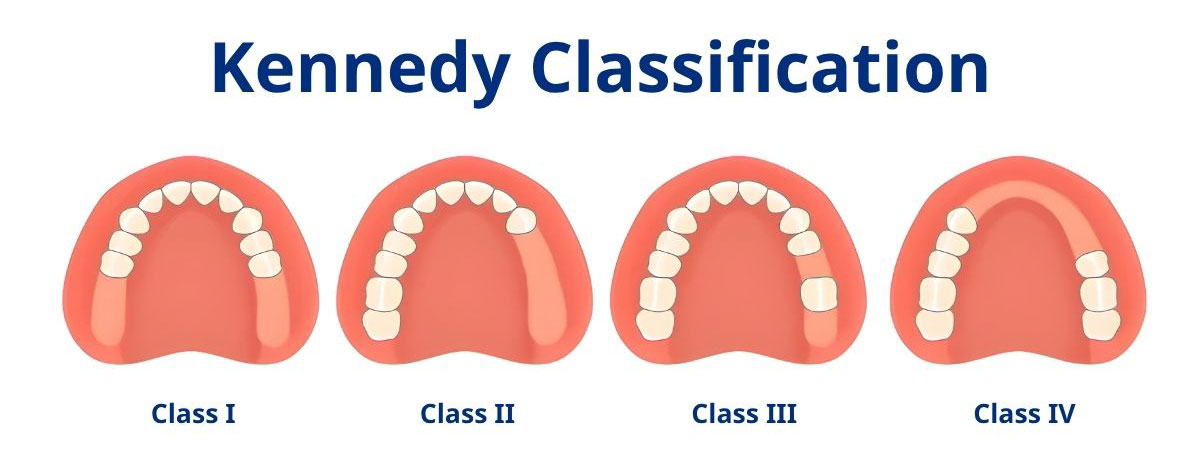
Core Classes
- Class I: Bilateral posterior edentulous areas (bilateral distal extension)
- Class II: Unilateral posterior edentulous area (unilateral distal extension)
- Class III: Unilateral bounded edentulous area (teeth remain anterior and posterior)
- Class IV: Single anterior edentulous area crossing the midline
Applegate’s Rules (Essentials)
- Classify after extractions that change posterior support.
- Ignore missing third molars unless serving as abutments.
- Ignore non-replaced second molars.
- The most posterior edentulous area determines the class.
- Additional edentulous areas are “modifications” by number.
- Class IV has no modifications.
Prevalence & Clinical Significance
- Class III is typically the most common overall; bounded spaces are frequent in both arches.
- Class I is often most common in older mandibular arches due to progressive posterior tooth loss.
- With age, Class I and II prevalence rises as support shifts from teeth to mucosa.
- Service planning implication: distal-extension cases require more adjustments and more frequent relines.
Biomechanics That Drive Design
Distal Extension (Classes I & II)
- Primary issue: rotation around a fulcrum line through the most posterior rests on abutments.
- Tissue compressibility under distal extension bases causes differential movement.
- Design levers: broad base coverage, indirect retainers, stress-releasing clasp assemblies (RPI/RPA), altered cast techniques, and implant assistance.
Tooth-Bounded (Class III)
- Tooth-supported frameworks with minimal tissue displacement.
- Focus on rigid connectors, ideal rest seats, and retentive undercuts to reduce torque on abutments.
Anterior Extension (Class IV)
- Aesthetics and leverage control dominate.
- Balanced clasping/attachments, indirect retention, and rotational path strategies minimize visibility and unseating forces.
Design Playbooks by Class
Kennedy Class I (Bilateral Distal Extension)
- Framework: Maxilla—anteroposterior palatal strap or full palatal coverage; Mandible—lingual bar if depth allows, otherwise lingual plate.
- Support & Retention: Mesial rests on distal abutments, guiding planes, RPI/RPA clasping, indirect retainers anterior to fulcrum line, broad bases with mesh, altered cast impressions.
- Implants: One implant per quadrant posteriorly often converts biomechanics toward Class III; use Locator/ball attachments.
- Risks mitigated: Ridge resorption, abutment overload, rotation under function.
Kennedy Class II (Unilateral Distal Extension)
- Framework: Emphasize cross-arch rigidity; connector selection mirrors Class I principles.
- Support & Retention: Indirect retainer on contralateral side, strategic clasping for balance and aesthetics, altered cast recommended.
- Implants: One to two implants on the distal-extension side reduce fulcrum rotation and improve stability.
Kennedy Class III (Bounded)
- Framework: Rigid major connector with conservative base coverage.
- Support & Retention: Rest seats on teeth bounding the span, conventional clasping (circumferential/Akers, cast clasps).
- Alternatives: Fixed prostheses or implants depending on span and abutment quality.
- Strengths: Fewer complications and high acceptance due to tooth support.
Kennedy Class IV (Anterior Across Midline)
- Aesthetics: Minimize visible clasps via rotational path designs or precision attachments.
- Biomechanics: Rigidity and indirect retention to counter anterior leverage.
- Alternatives: Implant-supported or resin-bonded fixed options when feasible.
Digital Workflows & Materials
Digital Impressions & CAD
- Accurate capture of undercuts, guiding planes, and ridge morphology.
- Virtual surveying for path of insertion and blockout planning.
- Rapid iterations and precise clinician–lab communication.
- Milled metal frameworks for consistent thickness and rigidity.
- Printed patterns for casting or direct-printed high-performance polymers (case dependent).
- PEEK frameworks: lightweight, metal-free; case selection is essential.
Denture Base & Teeth
- High-impact acrylics; milled or printed bases for controlled fit and reduced distortion.
- Attachment housings integrated with sufficient bulk and verified post-cure stability.
Implant-Assisted Kennedy Dentures (Classes I & II)
Rationale and Protocol
- Convert mucosa-dependent support into tooth/implant-bounded support.
- Reduce base movement and improve chewing efficiency and satisfaction.
- Place posterior implants near first molar/second premolar zones when feasible; verify restorative space early.
- Low-profile attachments (e.g., Locator) ease insertion/removal and hygiene.
Expected Outcomes
- Improved stability and retention, reduced ridge resorption, decreased abutment stress.
- Cost-effective alternative to fully fixed solutions for many patients.
Comparative Snapshot
| Kennedy Class | Support Pattern | Core Risks | Priority Design Elements |
|---|---|---|---|
| I (bilateral distal extension) | Teeth + mucosa | Rotation, abutment overload, ridge resorption | Broad bases, mesial rests, RPI/RPA, indirect retainers, altered cast; consider implants |
| II (unilateral distal extension) | Teeth + mucosa | Asymmetric rotation, off-axis loading | Cross-arch rigidity, indirect retainer opposite side, altered cast; consider implants |
| III (bounded) | Teeth | Minimal if well-designed | Rigid connector, ideal rests/guiding planes, conservative coverage; consider fixed options |
| IV (anterior across midline) | Teeth (posterior) | Aesthetics, leverage | Rigid connector, indirect retention, esthetic clasping/attachments; consider implants or fixed |
Maintenance & Long-Term Success
Clinical and Patient Protocols
- Professional recall every 6–12 months to assess fit, occlusion, tissue health, and clasp tension.
- Daily cleaning, clasp hygiene, removal at night, and case-specific insertion paths.
- Periodic relines for distal extensions; more frequent in Class I/II.
- Occlusal refinement for wear and tissue changes; periodontal maintenance for abutments.
QA & Risk Control for Clinics and Labs
Process Controls
- Verify classification after planned extractions; document modification spaces.
- Survey casts to define path of insertion and guide plane preparation.
- Impressions: altered cast or selective pressure for distal extensions; functional border molding.
- Framework try-in to confirm passive fit; re-survey if discrepancies appear.
- Implant attachments: confirm parallelism and housing seating; preserve acrylic bulk around housings.
- Documentation: photos, STL files, shade/contour preferences, clasp visibility notes.
Where XDENT LAB Fits
Capabilities and Collaboration
- FDA/ISO-aligned lab-to-lab capacity from Vietnam, specialized in Removable & Implant cases.
- Digital-first collaboration: survey analysis, CAD design previews, and documented QA.
- Validated SOPs for distal extension impressions, altered cast workflows, and implant attachment processing.
- Consistency, turnaround, and traceability tailored for group practices and DSOs seeking predictable outcomes.
Key Takeaways
Clinical and Operational Summary
- Kennedy Classification maps biomechanics to design choices and remains central to RPD planning.
- Distal extension cases benefit from broad base support, stress-release clasping, indirect retention, altered cast techniques, and often implants.
- Digital surveying, CAD/CAM frameworks, and modern materials enhance precision but do not replace biomechanical fundamentals.
- Maintenance and abutment care determine longevity as much as initial design.
- Partnering with an FDA/ISO-aligned lab like XDENT LAB streamlines complex cases and ensures repeatable quality across multi-site practices.
About XDENT LAB:
We are experts in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable, meet U.S. market standards - approved FDA & ISO. Founded in 2017, from local root to global reach, we scale with 2 Factories with over 100+ employees.

Our 5 Commitments Built on “Trusted. Commitment. Quality”
- Commit to 100% FDA-Approved Materials
- Commit to Large-Scale Manufacturing, high volume, remake rate < 1%.
- Commit to 2~3 days in lab (*digital file)
- Commit to Cost Savings 30%
- Commit to Best Price
XDENT LAB | A Trusted Lab-to-Lab Service from Vietnam
Share this post:





