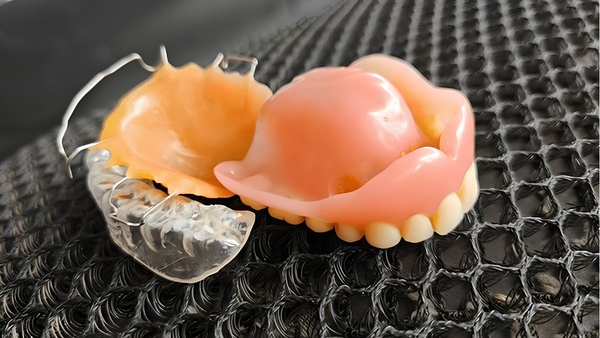
Light‑activated UDMA denture bases: flexural strength evidence, cure parameters, and QA. XDENT LAB’s FDA/ISO lab‑to‑lab workflow delivers consistent results.
Table of contents [Show]
- Overview
- Composition & Polymerization Essentials
- Processing Methods & Advanced Curing
- Physical, Mechanical & Aesthetic Properties
- Clinical & Laboratory Considerations
- Comparative Overview
- QA, Validation & Risk Control
- Implementation Playbook for Practices & Labs
- Research Trends & Future Directions
- Key Takeaways
Overview
Light-activated acrylic resins, typically based on UDMA chemistry, offer a modern alternative to conventional PMMA denture bases. They polymerize under visible light (≈400–500 nm), enabling controlled cure, reduced shrinkage, improved throughput, and strong cross-linked networks. For DSOs and high-volume practices in the dental industry, these resins can compress turnaround times and standardize quality—especially when paired with a lab-to-lab partner like XDENT LAB that meets FDA/ISO expectations.
Composition & Polymerization Essentials
Chemistry Highlights
Understanding the chemistry clarifies why these systems behave differently in the dental industry.
- Base monomer: Urethane dimethacrylate (UDMA) or related dimethacrylates with higher molecular weight than MMA for lower shrinkage and volatility.
- Photoinitiators: Camphorquinone with tertiary amines tuned to blue light for reliable radical formation.
- Cross-linkers: TEGDMA/HDMA and co-monomers to densify the network and elevate flexural performance.
- Fillers: Inorganic particles to modulate shrinkage, stiffness, and handling in the dental industry.
Polymerization Sequence
- Initiation: Blue light excites CQ; amines generate radicals.
- Propagation: Radical addition across methacrylate double bonds builds chains.
- Cross-linking: Multifunctional monomers form 3D networks for stiffness and solvent resistance.
- Termination: Radical quenching or mobility limits; post-cure deepens conversion in the dental industry.
Key upside: on-demand cure control, lower processing heat, and typically lower residual monomer than many self-cure systems used in the dental industry.
Processing Methods & Advanced Curing
Conventional Light-Cure Workflow
- Adapt sheets or putty to the master cast; control base thickness.
- Stage-light to lock margins; complete full light cycle per IFU (often 2–10 minutes).
- Post-cure for mass/opaque areas; then finish and polish.
Net effect: fewer flasking variables and leaner handling overhead in the dental industry.
Advanced Approaches
- Argon ion laser cure: Higher irradiance and depth of cure for thick sections; evaluate heat management and equipment ROI in the dental industry.
- Variable exposure protocols: Intensity and time tuning to optimize degree of conversion and flexural strength.
- DLP/LCD 3D printing: Digital light processing enables additively manufactured bases and hybrid flows, broadening indications in the dental industry.
Physical, Mechanical & Aesthetic Properties
Flexural Behavior
- Many studies report higher flexural strength and modulus vs. some PMMAs and polycarbonate-reinforced options when cure is optimized.
- Exposure time, irradiance, and post-cure strongly affect outcomes in the dental industry.
Dimensional Stability
- Lower polymerization shrinkage than MMA systems supports better base adaptation and retention.
- Water sorption and thermal cycling still influence long-term fit; monitor with QA checks in the dental industry.
Color Stability
- Eclipse-type systems often show better resistance to staining vs. traditional heat-cure resins, though tea and chromogens still challenge surfaces over time in the dental industry.
Other Performance Factors
- Impact strength: Frequently improved with optimized cross-linking and fillers.
- Surface hardness: Generally higher; enhances wear resistance and polishing outcomes.
- Fatigue resistance: Cross-linked networks support cyclic durability for high-function patients in the dental industry.
- Bond to teeth: Surface treatments and compatible bonding resins are crucial for tooth–base integrity.
Clinical & Laboratory Considerations
Advantages
- Processing efficiency: No water-bath cycles; predictable, on-demand curing.
- Reduced residual monomer: Potentially lower irritation risk.
- Strong, cross-linked network: Better mechanical resilience in daily use across the dental industry.
- Aesthetic longevity: Improved chromatic stability for many systems.
Limitations
- Equipment costs: Specialized light boxes or curing chambers and, where used, laser units.
- Thickness constraints: Ensure sufficient light energy for deep sections in the dental industry.
- Repairs and relines: Cross-linked matrices may need primers, surface conditioning, or specialized kits.
- Learning curve and IFU discipline: Small deviations can undercut conversion.
Clinical Applications
- Complete dentures: Efficient base fabrication with reliable adaptation.
- Partial dentures and hybrid frameworks: Selective reinforcement and controlled cure in the dental industry.
- Implant-supported overdentures: Precision fit and stable occlusion schemes; verify conversion around housings.
- Repairs and modifications: Protocol-dependent success; follow manufacturer chemistry.
Comparative Overview
Material Selection at a Glance
| Material | Processing | Strength/Fit | Color Stability | Repairability |
|---|---|---|---|---|
| Heat-cure PMMA | Flask, pack, heat | Good; shrinkage control depends on cycle | Moderate | Straightforward |
| Self-cure PMMA | Cold cure | Moderate; higher residual monomer | Lower | Easy; porosity risk |
| Light-activated UDMA | Visible-light cure | High when fully cured; low shrinkage | Often higher | Protocol-sensitive |
| DLP-printed resins | Layered light cure | Improving; high design precision | Improving | System-specific |
Light-activated UDMA balances speed, fit, and mechanical performance for many labs in the dental industry, provided curing protocols are validated.
QA, Validation & Risk Control
Checklist for Regulated Workflows
- Verify radiometer output: Match device irradiance to IFU; re-check quarterly.
- Build cure maps: Record exposure vs. base thickness and shade for your unit.
- Degree of conversion checks: FTIR where available or proxy rub tests in the dental industry.
- Water sorption and thermal cycling: Internal controls to forecast fit drift.
- Bonding protocol SOP: Standardize tooth surface treatment and resin compatibility.
- MDR/FDA alignment: Track lots, IFUs, and batch records; retain device history.
Implementation Playbook for Practices & Labs

Workflow Design
- Digital intake: Scan verification and base thickness planning.
- Staged light: Margin lock, full cure, and mandatory post-cure windows.
- Finishing SOPs: Uniform polishing sequence to control gloss and stain pickup in the dental industry.
When to Choose Light-Activated Systems
- Tight turnaround cases where flasking overhead is a bottleneck.
- Patients with previous tissue sensitivity related to residual monomer.
- Implant overdentures needing precise adaptation and resilient bases in the dental industry.
- Aesthetic longevity prioritized for tea or coffee-heavy diets.
XDENT LAB Positioning
XDENT LAB delivers FDA/ISO-aligned lab-to-lab capacity from Vietnam with U.S. standardization. Our Removable and Implant specialization, documented QC, and validated curing profiles provide the consistency demanded by the dental industry.
Research Trends & Future Directions
Material Innovations
- Monomer innovation for toughness without brittleness and lower eluables.
- Antimicrobial integration to modulate biofilm without compromising biocompatibility.
- Self-healing chemistries to resist crack propagation and extend service life in the dental industry.
Processing Advancements
- Optimized light-curing units with wavelength distribution, intensity, and beam homogeneity for complete conversion.
- Digital workflow integration: Impression, design, and manufacturing alignment.
- DLP chemistry tuning: Higher conversion at lower dose for faster, deeper cures in the dental industry.
- Hybrid lines: Subtractive–additive blends with automated QA and in-line dosimetry.
Research Needs
- Long-term clinical trials comparing light-activated and conventional alternatives.
- Aging and degradation mechanisms in the oral environment.
- Validated repair and reline protocols for cross-linked matrices.
- Biofilm formation studies and sustainable formulations relevant to the dental industry.
Key Takeaways
Summary for Decision-Makers
- Light-activated UDMA systems deliver controlled cure, lower shrinkage, and robust mechanicals—a strong fit for standardized, time-sensitive workflows in the dental industry.
- Outcomes depend on irradiance, exposure time, post-cure, and disciplined bonding protocols.
- For practices seeking predictable quality at scale, partnering with an FDA/ISO-aligned lab like XDENT LAB reduces variance and speeds delivery while meeting documentation expectations in the dental industry.
About XDENT LAB:
We are experts in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable, meet U.S. market standards - approved FDA & ISO. Founded in 2017, from local root to global reach, we scale with 2 Factories with over 100+ employees.

Our 5 Commitments Built on “Trusted. Commitment. Quality”
- Commit to 100% FDA-Approved Materials
- Commit to Large-Scale Manufacturing, high volume, remake rate < 1%.
- Commit to 2~3 days in lab (*digital file)
- Commit to Cost Savings 30%
- Commit to Best Price
XDENT LAB | A Trusted Lab-to-Lab Service from Vietnam
Share this post: