Comprehensive guide to chemical‑cured (self‑cure) acrylic resin for denture bases: composition, polymerization, mechanical performance, shrinkage and residual monomer, reinforcement (glass fiber, wire), clinical indications (repairs, interim, ortho), vs. heat‑cure, and ISO/FDA‑aligned QA.
Table of contents [Show]
- Overview
- Composition & Polymerization
- Mechanical Properties
- Dimensional Stability & Residual Monomer
- Reinforcement Strategies
- Clinical & Laboratory Applications
- Comparative Analysis: Chemical-Cure vs. Heat-Cure
- Process Controls & QA (ISO/FDA Aligned)
- Recent Innovations & Future Directions
- Practical Playbook for Dental Practices
- XDENT LAB Approach (Lab-to-Lab, FDA/ISO Compliant)
- Key Takeaways
Overview
Chemical-cured acrylic resins (also called cold-cure, self-cure, or auto-polymerizing PMMA) polymerize at room temperature via chemical activation rather than heat. That difference enables rapid chairside use and repairs but typically yields lower conversion, higher residual monomer, and reduced mechanical performance versus heat-cured PMMA. For dental practices and labs, the strategic use case is clear: deploy chemical-cure for repairs, interim devices, and orthodontic appliances, while applying validated protocols, reinforcements, and post-treatments to mitigate known weaknesses within FDA/ISO-aligned workflows.
Composition & Polymerization
Chemical-cured PMMA employs a two-part system that activates without external heat.
Chemical Composition
Powder: Pre-polymerized PMMA beads with benzoyl peroxide initiator.
Liquid: MMA monomer with tertiary amine activator (e.g., dimethyl-p-toluidine).
Optional modifiers: pigments, opacifiers, plasticizers, fibers, or fillers for reinforcement.
Polymerization Mechanism
Initiation: Amine activates benzoyl peroxide to create free radicals.
Propagation: MMA converts to PMMA via chain growth.
Termination: Combination or disproportionation.
Notes: Exothermic set; room-temperature cure often leads to lower conversion and higher residual monomer than heat-cure.
Mechanical Properties
Chemical-cured PMMA is suitable for repairs and interim devices but is typically inferior to heat-cure for definitive bases unless reinforced.
Flexural Performance
Baseline flexural strength is commonly around 75–80% of heat-cured values at room temperature.
Improvements with:
Slightly elevated polymerization temperature (e.g., 40–55°C in a pressure/heat pot).
Extended polymerization time per manufacturer instructions.
Pressure polymerization (approximately 2–3 bar) to reduce porosity.
Impact Strength & Fatigue
Lower impact and fatigue resistance than heat-cured PMMA.
Frequent failure sites: repair interfaces, thin flanges, and regions near notches or stress concentrators.
Use reinforcement and proper joint design to enhance durability.
Dimensional Stability & Residual Monomer
Accuracy and biocompatibility depend on managing shrinkage and conversion.
Shrinkage & Fit
Higher polymerization shrinkage than heat-cure increases risk of misfit if used for full bases.
Best suited for localized repairs or interim devices.
Mitigation: pressure polymerization, correct powder-liquid ratios, bench rest to relieve internal stresses.
Residual Monomer & Biocompatibility
Higher residual monomer can reduce strength, increase water sorption/solubility, and irritate tissues.
Mitigation:
Post-polymerization heat/pressure cycles to raise conversion.
Rinse and brief water storage prior to delivery.
Use reputable, ISO 20795-1 conforming materials.
Reinforcement Strategies
Reinforcement transforms a quick-setting material into a more robust repair system.
Fiber Reinforcement
Glass fibers (silanized; pre-impregnated mats/rovings) provide the largest gains in flexural strength and stiffness.
Ensure proper wetting and alignment along tensile zones.
Polyethylene (UHMWPE) fibers enhance impact and fatigue; surface treatment improves bonding.
Stainless steel or cobalt-chromium wires effectively bridge fracture lines and high-stress zones.
Embed fully with adequate acrylic coverage to prevent stress concentration.
Particulate Fillers
Selected nano/micro fillers (e.g., ZrO2, Al2O3, SiO2) can improve hardness and modulus.
Excessive loading may cause embrittlement.
Clinical & Laboratory Applications
Use chemical-cured resins where speed and localized modification are advantageous.
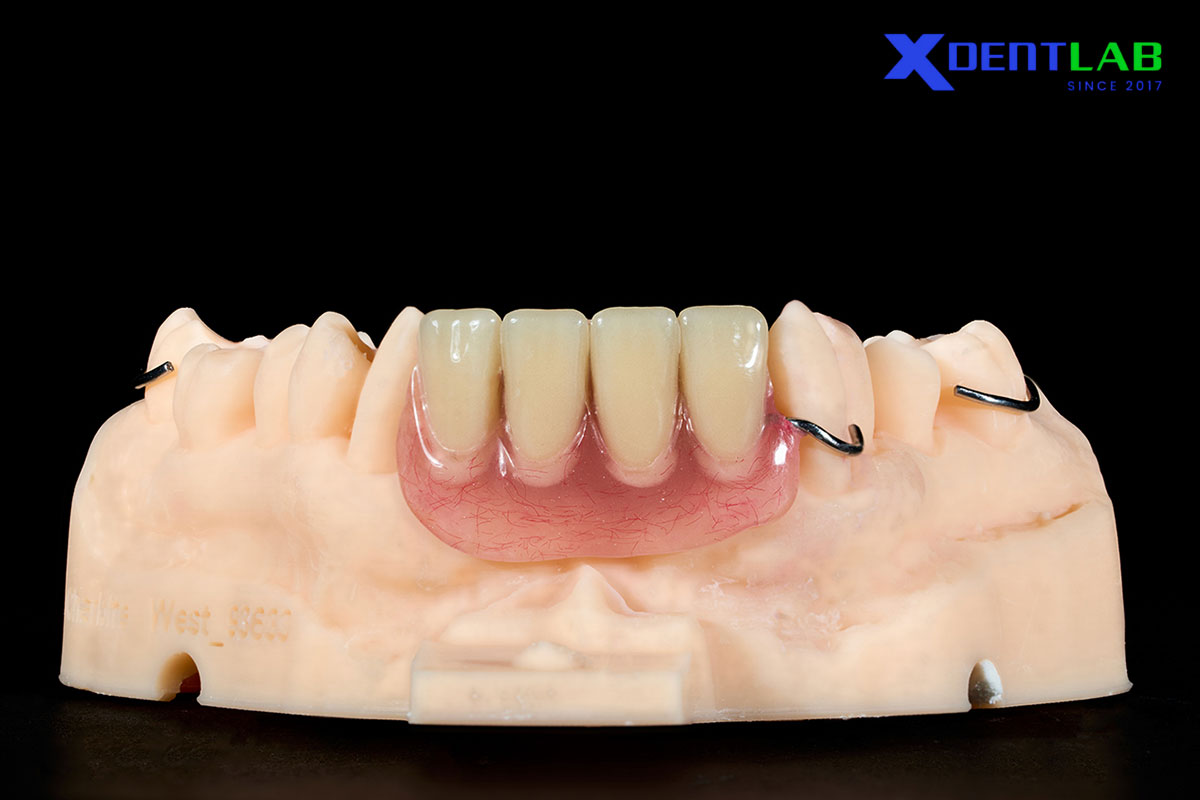
Denture Repairs
Indications: fracture repair, tooth replacement, clasp/extension additions.
Best practices:
Joint design: bevel/scarf with broad overlap.
Surface treatments: air abrasion (e.g., 50 µm Al2O3), MMA wetting, or compatible primers.
Pressure pot polymerization to minimize porosity.
Consider glass fiber or wire reinforcement across the fracture line.
Post-repair heat/pressure cycle to improve conversion.
Immediate dentures, transitional partials, surgical stents.
Rapid turnaround and lower cost; plan definitive replacement with heat-cure or milled PMMA.
Orthodontic & Adjunctive Appliances
Hawley retainers, habit appliances, splints.
Room-temperature cure allows safe integration of wires and components.
Comparative Analysis: Chemical-Cure vs. Heat-Cure
Strength & Fatigue
Chemical-cure: lower baseline flexural and impact performance.
Heat-cure: higher conversion and toughness; preferred for definitive bases.
Fit & Dimensional Stability
Chemical-cure: higher polymerization shrinkage and greater risk of misfit.
Heat-cure: better stability; injection molding improves adaptation further.
Residual Monomer & Color Stability
Chemical-cure: higher residual monomer and water sorption → greater risk of early irritation and discoloration.
Heat-cure: lower residual monomer; superior long-term color retention.
Process Controls & QA (ISO/FDA Aligned)
Consistent outcomes require validated processes and documentation.

Material Handling
Follow manufacturer ratios and working/set times.
Control room temperature and humidity to stabilize kinetics.
Polymerization Controls
Use a pressure pot (approximately 2–3 bar) and warm water when indicated to reduce porosity and raise conversion.
Avoid deflasking or trimming before full set.
Surface Preparation & Bonding
Ensure complete dewaxing and contamination control.
Air abrasion plus MMA wetting or approved bonding agents at repair interfaces.
Post-Processing
Finish and polish to surface roughness Ra < 0.2 µm.
Rinse and brief water storage before delivery to reduce residual monomer.
Documentation
Track resin lots, cure parameters, and inspection checkpoints.
Verify conformance to ISO 20795-1 where applicable.
Recent Innovations & Future Directions
Pour-Type Auto-Polymerizing Resins
Reformulations and controlled pour techniques improve conversion and flexural values.
Best results with pressure and mild heat assistance.
Surface Coatings & Treatments
Light-cured coatings can reduce monomer leach and enhance gloss.
Plasma or chemical activation improves bonding in multi-material assemblies.
Practical Playbook for Dental Practices
Reserve chemical-cure for repairs, additions, interim prostheses, and orthodontic/auxiliary appliances.
Choose heat-cure injection or milled PMMA for definitive full/partial bases.
When repairing: use scarf joints, sandblast and MMA-wet, reinforce across high-stress paths, and employ pressure polymerization with optional post-repair heat.
Provide patient guidance on gentle initial use, proper cleaning, and avoiding hot water; schedule follow-up for polish and interface checks.
XDENT LAB Approach (Lab-to-Lab, FDA/ISO Compliant)
Use-Case Triage
Chemical-cure for time-sensitive repairs and interim devices.
Heat-cure injection or milled PMMA for definitive durability and fit.
Reinforcement Protocols
Silanized glass fiber or wire integration with validated joint geometries.
Quality System
Material lot traceability, pressure pot logs, and surface-prep checklists.
ISO-aligned inspection for porosity, bond integrity, and surface finish.
Communication Artifacts
Standardized Rx forms, repair design diagrams, and turnaround SLAs for predictable outcomes.
Key Takeaways
Chemical-cured acrylic resins excel in speed and convenience for repairs and interim solutions but lag heat-cured PMMA in strength, stability, and color retention.
Reinforcements, pressure polymerization, and disciplined surface treatments significantly improve repair performance and patient comfort.
A hybrid strategy—chemical-cure for repairs/interim, heat-cure or milled for definitive—delivers efficiency, compliance, and longevity in modern lab-to-lab workflows.
XDENT LAB is an expert in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable & Implant, meeting U.S. market standards – approved by FDA & ISO. Founded in 2017, XDENT LAB has grown from local root to global reach, scaling with 2 factories and over 100 employees.. Our state-of-the-art technology, certified technicians, and commitment to compliance make us the trusted choice for dental practices looking to ensure quality and consistency in their products.
Our commitments are:
100% FDA-Approved Materials.
Large-Scale Manufacturing, high volume, remake rate < 1%.
2~3 days in lab (*digital file).
Your cost savings 30%.
Uninterrupted Manufacturing 365 days a year.
Contact us today to establish a strategy to reduce operating costs.
--------❃--------
Vietnam Dental Laboratory - XDENT LAB
🏢 Factory 1: 95/6 Tran Van Kieu Street, Binh Phu Ward, Ho Chi Minh City, Vietnam
🏢 Factory 2: Kizuna 3 Industrial Park, Can Giuoc Commune, Tay Ninh Province, Vietnam
☎ Hotline: 0919 796 718 📰 Get detailed pricing
Share this post: