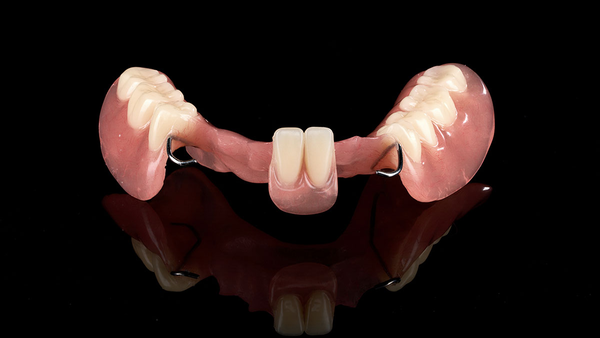
Modern preventive dentistry explained: evidence-based strategies, risk-based recalls, fluoride and sealants, SDF and remineralization, and community programs. Explore emerging tech (salivary diagnostics, remote monitoring), precision prevention, and oral–systemic integration, with practical SOPs and FDA/ISO-aligned workflows from XDENT LAB for consistent, cost-effective outcomes.
Table of contents [Show]
- Overview
- Evidence-Based Preventive Dentistry
- Key Preventive Strategies
- Risk Assessment & Personalized Prevention
- Nonrestorative Caries Management
- Public Health & Integration with Primary Care
- Population-Specific Strategies
- Cost-Effectiveness & Policy
- Challenges & Implementation Gaps
- Future Directions
- A Modern Framework for Prevention
- Evidence-Based Chairside Playbook (XDENT LAB)
- Key Takeaways
Overview
Preventive dentistry centers on stopping disease before it starts—reducing caries, periodontal disease, and oral cancer risk through evidence-based care, patient education, and risk-driven recall. Guided by ADA and CDC frameworks, prevention delivers the strongest return on health and cost when protocols are individualized and consistently implemented. This analysis distills core strategies, risk assessment, public health integrations, and pragmatic rollout steps for practices partnering with XDENT LAB.
Evidence-Based Preventive Dentistry
Evidence-based dentistry (EBD) integrates best-available research, clinical judgment, and patient preferences to select preventive interventions with the highest value for each individual.
EBD Framework
Systematic assessment: prioritize high-quality guidelines, RCTs, and systematic reviews.
Clinical expertise: calibrate techniques, recall intervals, and adjuncts to risk and feasibility.
Patient factors: align with health history, behavior readiness, and access constraints.
Levels of Prevention
Primary: water fluoridation, sealants, home fluoride, oral hygiene training.
Secondary: risk-based recalls, caries/periodontal screening, radiography per evidence.
Tertiary: minimally invasive treatments to limit disability and restore function.
Key Preventive Strategies
Fluoride Interventions
Community water fluoridation: ~25% caries reduction across ages; high-value public health measure.
In-office fluoride: varnish/gels for high-risk patients; underutilized in adults and older adults.
Home fluoride: twice-daily fluoride toothpaste, risk-based rinses/prescription pastes.
Dental Sealants
Effectiveness: ≥80% caries reduction on occlusal surfaces in first 2 years with proper technique.
Programs: school-based sealant initiatives improve equity and cost-effectiveness.
Implementation gap: underused in low-risk groups despite favorable evidence and safety.
Oral Hygiene & Behavioral Interventions
Mechanical plaque control: twice-daily brushing with fluoride; daily interdental cleaning.
Behavior change: motivational interviewing and skills training outperform advice alone.
Risk counseling: diet, tobacco, alcohol, and systemic factors tailored to readiness and context.
Diet & Nutrition Counseling
Sugars: reduce frequency of fermentable carbohydrate intake; manage snacking patterns.
Protective nutrients: support periodontal and mucosal health (e.g., calcium, vitamin D, antioxidants).
Personalization: align guidance with cultural preferences and socioeconomic realities.
Regular Exams & Professional Care
Recalls: individualized intervals by risk; not one-size-fits-all six-month schedules.
Prophylaxis: align frequency to periodontal risk rather than routine semiannual default for all.
Radiographs: interval selection guided by caries/periodontal risk and prior findings.
Risk Assessment & Personalized Prevention
Caries Risk Assessment
Risk inputs: past caries, diet, fluoride exposure, saliva flow, hygiene, socioeconomic factors.
Tools: CAMBRA and ADA forms standardize scoring and recommended interventions.
Risk-based care: intensify fluoride, sealants, and recalls for high-risk; de-intensify for low-risk.
Periodontal Risk Assessment
Risk inputs: smoking, diabetes, genetics, prior periodontitis, hygiene level, systemic status.
Protocols: tailored maintenance frequency, adjunct antimicrobials, and focused self-care coaching.
Nonrestorative Caries Management
Silver Diamine Fluoride (SDF)
Indications: arrest active lesions where conventional care is limited by access or tolerance.
Considerations: lesion selection, aesthetic impact, informed consent, and follow-up.
Remineralization Strategies
High-fluoride agents, calcium phosphate technologies, and bioactive materials for early lesions.
Decision factors: lesion activity, salivary status, patient adherence, and cost.
Public Health & Integration with Primary Care

Community-Based Programs
Water fluoridation, school sealants, fluoride rinses, and school toothbrushing programs.
Targeted outreach to rural, low-income, elderly, and disability communities.
Medical-Dental Collaboration
Screening and fluoride varnish in primary care for children and at-risk adults.
Shared risk factor management for diet, tobacco, and alcohol across care teams.
Population-Specific Strategies
Children & Adolescents
Dental home by age 1; anticipatory guidance for caregivers.
Sealants on erupting molars; age-appropriate fluoride and hygiene coaching.
Adults
Risk-based recalls, tailored hygiene (especially around restorations/exposed roots).
Lifestyle counseling and caries/periodontal risk mitigation.
Older Adults
Xerostomia management, root caries prevention with high-fluoride agents.
Strategies to maintain mastication and nutrition; caregiver-supported hygiene where needed.
Cost-Effectiveness & Policy
Economic Evidence
Prevention reduces restorative and emergency costs; strong ROI for fluoridation and sealants.
Broader benefits: fewer school/work absences and better quality of life.
Coverage & Incentives
Expand insurance for preventive services; value-based models reward prevention outcomes.
Fund school and community programs with demonstrated returns.
Challenges & Implementation Gaps
Financial limits, provider shortages, and geographic disparities.
Cultural, language, and health literacy hurdles.
Practice & Patient Adherence
Inconsistent adoption of risk-based recalls and sealant/fluoride protocols.
Behavioral adherence at home requires ongoing coaching and feedback loops.
Future Directions
Technology & Precision Prevention
Salivary diagnostics, microbiome-informed care, and remote monitoring.
Personalized prevention pathways integrating genetics and systemic risk.
Oral–Systemic Integration
Coordinated management of shared risk factors tied to diabetes, CVD, and pregnancy outcomes.
Care models that embed dental prevention within primary care and community health.
A Modern Framework for Prevention
Upstream Determinants & Equity
Policies addressing social and environmental drivers of oral disease.
Life-course strategies that adapt across developmental stages.
Evidence-Based Chairside Playbook (XDENT LAB)
XDENT LAB supports U.S.-standard preventive outcomes with standardized, auditable workflows suitable for dental practices focused on quality and consistency.
Risk-Based SOPs
Adopt CAMBRA/ADA forms; embed decision support in EHR for recalls, radiographs, and fluoride/sealant indications.
Fluoride & Sealant Protocols
Define high-risk indications for varnish and prescription fluoride; standardize sealant selection and isolation method (including GI/RMGI in moisture-challenged cases).
Training & QA
Team calibration on technique; batch and IFU traceability; periodic audits for compliance (FDA/ISO aligned).
Patient Engagement
Brief, scripted behavior-change counseling; printed/portal instructions to reinforce home care and follow-ups.
Key Takeaways
Prevention works best when personalized by risk and delivered consistently across visits and teams.
Fluoride, sealants, risk-based recalls, and behavioral counseling are the highest-value levers.
Public health programs amplify equity and ROI; integration with primary care expands reach.
XDENT LAB’s standardized, FDA/ISO-aligned processes help practices operationalize prevention reliably and at scale.
XDENT LAB is an expert in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable & Implant, meeting U.S. market standards – approved by FDA & ISO. Founded in 2017, XDENT LAB has grown from local root to global reach, scaling with 2 factories and over 100 employees.. Our state-of-the-art technology, certified technicians, and commitment to compliance make us the trusted choice for dental practices looking to ensure quality and consistency in their products.

Our commitments are:
100% FDA-Approved Materials.
Large-Scale Manufacturing, high volume, remake rate < 1%.
2~3 days in lab (*digital file).
Your cost savings 30%.
Uninterrupted Manufacturing 365 days a year.
Contact us today to establish a strategy to reduce operating costs.
--------❃--------
Vietnam Dental Laboratory - XDENT LAB
🏢 Factory 1: 95/6 Tran Van Kieu Street, Binh Phu Ward, Ho Chi Minh City, Vietnam
🏢 Factory 2: Kizuna 3 Industrial Park, Can Giuoc Commune, Tay Ninh Province, Vietnam
☎ Hotline: 0919 796 718 📰 Get detailed pricing
Share this post: