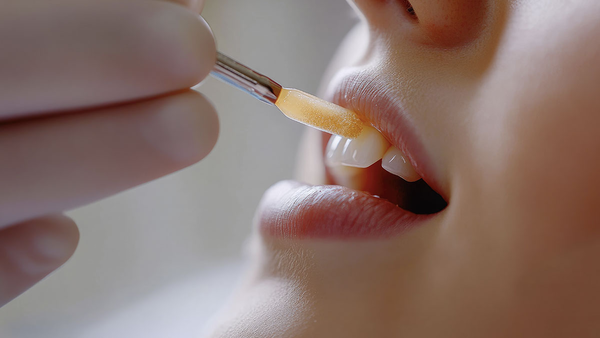
What bioactive sealants do and how they work: ion release, remineralization, clinical indications, and technique tips for high‑risk and orthodontic patients.
Table of contents [Show]
Bioactive sealants go beyond a physical barrier. They are formulated to release ions—fluoride, calcium, and phosphate—that support remineralization while sealing pits and fissures. Compared with traditional resin sealants, their value is most apparent in high-risk patients, around orthodontic appliances, and in preventive programs where retention and ion exchange matter. This article provides a structured overview of composition, properties, indications, comparisons, and implementation within FDA/ISO-aligned workflows, including how XDENT LAB supports predictable outcomes across clinics.
Composition and Mechanism of Action
Bioactive sealants blend resin chemistry with ion-releasing fillers to create a protective, therapeutic interface on occlusal surfaces.
Core Components
- Resin matrix: Methacrylate-based systems designed for light curing, flow into fissures, and micromechanical retention.
- Bioactive fillers: Ion-leachable (bioactive glass or fluoroaluminosilicate) particles that release fluoride, calcium, and phosphate.
- Additives: Optional antimicrobial agents and wetting/flow modifiers to enhance handling and therapeutic efficacy.
How They Work
- Immediate function: After enamel conditioning and light curing, the resin establishes a micromechanical seal.
- Ongoing bioactivity: Salivary exposure drives ion exchange—fluoride, calcium, and phosphate diffuse to enamel, supporting remineralization and buffering acids.
- Clinical implication: Compared with traditional sealants, bioactive options add a therapeutic layer that may reduce lesion progression in high-caries-risk patients.
Properties That Influence Clinical Outcomes
Performance depends on retention, wear, and biocompatibility alongside sustained ion release.
Mechanical and Handling Characteristics
- Compressive strength: Typically comparable to conventional sealants (approximately 100–200 MPa).
- Flexural strength: Commonly above 50 MPa, adequate for occlusal service.
- Wear resistance: Similar to resin sealants for long-term occlusal function when isolation and technique are sound.
- Bond strength: Driven by enamel conditioning and adhesive system compatibility; follow product IFUs.
- Viscosity and flow: Thixotropic behavior for deep fissure penetration without slumping.
Bioactivity and Clinical Effects
- Ion release: Fluoride plus calcium/phosphate support remineralization and reduce demineralization at margins.
- Recharge potential: Many formulations absorb fluoride from toothpaste/varnish and re-release over time.
- Antimicrobial traits: Some include agents that modestly reduce cariogenic biofilm formation.
- Biocompatibility: Favorable profiles; transient pH shifts stabilize after polymerization.
Indications, Contraindications, and Technique
Case selection and consistent technique maximize the preventive benefits of bioactive sealants.
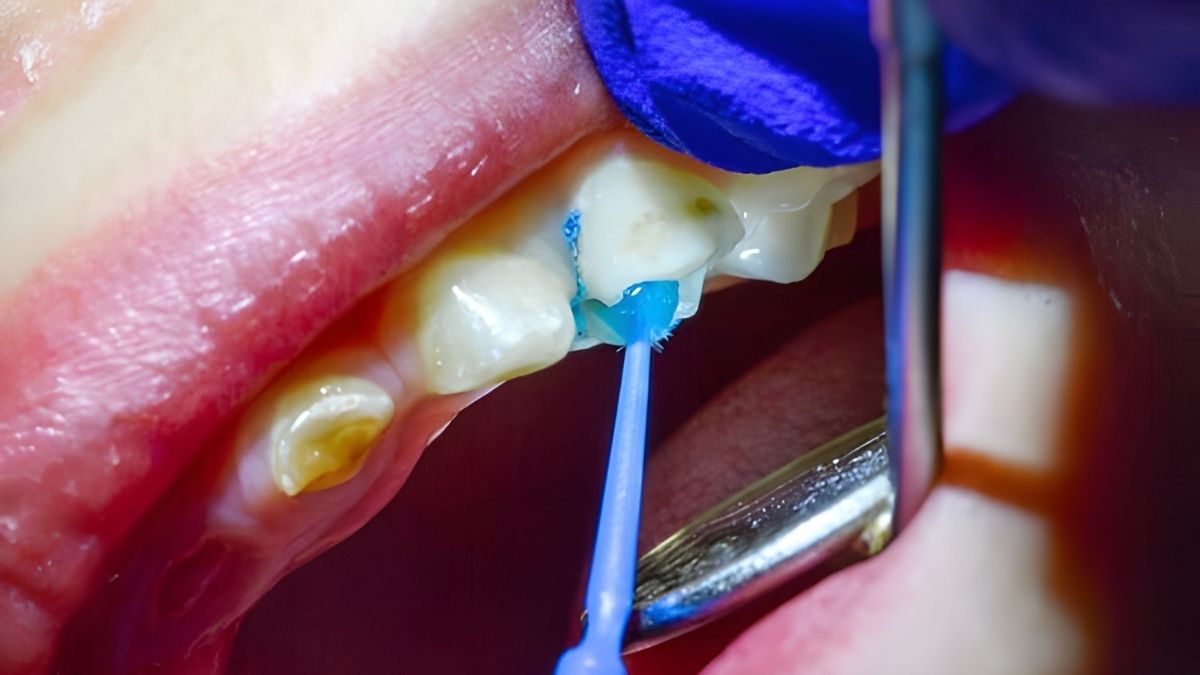
Primary Indications
- Pit and fissure sealing for children, adolescents, and high-risk adults.
- Caries management of early non-cavitated lesions (ICDAS 1–2) within minimally invasive care.
- Orthodontic applications around brackets to reduce white-spot lesion risk.
- Adjunctive prevention for special-needs and xerostomic patients with elevated caries risk.
Contraindications
- High-stress restorative needs: Class II load-bearing lesions; choose composite or RMGIC pathways.
- Extensive structural defects: Severe enamel hypoplasia or retention-poor surfaces.
- Poor isolation: When reliable bonding cannot be achieved; consider GIC alternatives or interim measures.
Technique Pearls
- Isolation: Rubber dam or meticulous retraction; moisture control is the primary determinant of retention.
- Enamel conditioning: Etch with phosphoric acid or use recommended primers per IFU; rinse and dry to a chalky enamel appearance when indicated.
- Placement: Scrub sealant into fissures; avoid puddling; gentle air thinning; light-cure as directed; verify coverage and absence of voids.
- Occlusion and finish: Check contacts; remove excess; confirm margins; re-evaluate at recalls for integrity and re-seal if needed.
- Prevention synergy: Schedule fluoride varnish and recommend high-fluoride toothpaste to leverage recharge potential.
Comparative Analysis
The table below helps differentiate bioactive sealants from traditional resin and glass ionomer options for faster decision-making.
| Sealant Type | Setting & Adhesion | Ion Release | Retention & Wear | Moisture Tolerance | Best Use Cases |
|---|---|---|---|---|---|
| Traditional resin sealant | Light-cure; micromechanical retention after etch | Fluoride (varies; often limited) | High with excellent isolation | Low; technique-sensitive | Standard pit and fissure sealing with ideal isolation |
| Glass ionomer (GIC) sealant | Acid–base set; chemical adhesion | High fluoride; strong recharge | Lower wear; faster material loss | Higher tolerance during placement | Interim sealing, compromised isolation, high-risk cases |
| Bioactive resin sealant | Light-cure; micromechanical adhesion via etch/prime | Fluoride + calcium/phosphate; recharge potential | Comparable to resin; added therapeutic benefit | Slightly more forgiving; still technique-sensitive | High-risk occlusal surfaces, around brackets, ICDAS 1–2 lesions |
Key takeaway: Bioactive sealants preserve the retention profile of resin-based systems while adding clinically meaningful ion exchange—especially valuable in high-risk and orthodontic contexts.
Decision Pathway for Busy Clinics
Use a standardized algorithm to reduce variability and improve outcomes across providers.
- Caries risk high? Favor bioactive or GIC sealants; if isolation is reliable, choose bioactive resin first-line.
- Isolation quality? Excellent → bioactive or traditional resin; compromised → consider GIC as interim, then upgrade.
- Lesion status? Non-cavitated (ICDAS 1–2) → bioactive sealant with monitoring; cavitated → minimally invasive restoration pathway.
- Orthodontic appliances? Apply bioactive sealant around brackets for white-spot prevention.
- Recall plan? Schedule re-evaluation; re-seal as needed; incorporate fluoride varnish cadence for recharge.
Recent Developments and Future Directions
- Enhanced ion-release profiles with improved calcium/phosphate kinetics and sustained fluoride without sacrificing wear resistance.
- Nanofiller systems for better fissure penetration and polish retention with lower viscosity.
- Antimicrobial integration (e.g., quaternary ammonium/biomimetic peptides) under investigation to suppress biofilm.
- Color-change cure indicators for visual confirmation of complete set in deep fissures.
- Digital synergy: aligning sealant selection with risk scoring from practice analytics and AI caries detection systems.
Implementation with XDENT LAB (FDA/ISO)
XDENT LAB supports dental practices seeking reliability and scale through standardized, FDA/ISO-aligned protocols for preventive materials, including bioactive sealants.
How XDENT LAB Standardizes Outcomes
- Validated materials library: FDA/ISO-aligned bioactive sealant SKUs with batch traceability and integrated IFUs.
- Protocol sheets by indication: Etch/adhesive pairing, curing times, and isolation checklists tailored to pediatric, orthodontic, and high-risk adult workflows.
- Chairside–lab checklists: Map risk status, isolation quality, and lesion stage to material choice; capture images for audit and training.
- Recharge workflows: Fluoride varnish cadence and at-home recommendations embedded in recall templates.
- Feedback loop: Retention audits inform continuous refinement across multi-site groups.
Where It Fits in Your Service Mix
- School-based and pediatric programs: fast, standardized placement with high recall capture.
- Orthodontic prevention packages: around-bracket sealing pathways to reduce white-spot incidence.
- Geriatric and xerostomia protocols: protective sealing for at-risk occlusal surfaces with remineralization support.
Practical Takeaways
- Bioactive sealants combine resin retention with therapeutic ion release for high-risk occlusal surfaces and around orthodontic brackets.
- Outcomes depend on isolation quality, enamel conditioning, and consistent recall for inspection and re-seal.
- Adopt a decision tree linking caries risk and isolation to material selection, with documented lot numbers and curing parameters.
- With FDA/ISO-aligned SOPs, XDENT LAB helps clinics deploy bioactive sealants as part of a preventive ecosystem that is documented, scalable, and patient-centric.
XDENT LAB is an expert in Lab-to-Lab Full Service from Vietnam, with the signature services of Removable & Implant, meeting U.S. market standards – approved by FDA & ISO. Founded in 2017, XDENT LAB has grown from local root to global reach, scaling with 2 factories and over 100 employees.. Our state-of-the-art technology, certified technicians, and commitment to compliance make us the trusted choice for dental practices looking to ensure quality and consistency in their products.
Our commitments are:
100% FDA-Approved Materials.
Large-Scale Manufacturing, high volume, remake rate < 1%.
2~3 days in lab (*digital file).
Your cost savings 30%.
Uninterrupted Manufacturing 365 days a year.
Contact us today to establish a strategy to reduce operating costs.
--------❃--------
Vietnam Dental Laboratory - XDENT LAB
🏢 Factory 1: 95/6 Tran Van Kieu Street, Binh Phu Ward, Ho Chi Minh City, Vietnam
🏢 Factory 2: Kizuna 3 Industrial Park, Can Giuoc Commune, Tay Ninh Province, Vietnam
☎ Hotline: 0919 796 718 📰 Get detailed pricing
Share this post: